Emergency Medicine Billing Services
Emergency medicine billing is one of the most demanding and fast-paced specialties, driven by high patient volumes, diverse acuity levels, rapid clinical decision-making, complex documentation, split/shared visit requirements, and strict payer scrutiny for critical care coding. With unpredictable case types, frequent diagnostic add-ons, and time-sensitive reporting, ED practices often face challenges maintaining billing accuracy and steady cash flow.
MedVoice provides comprehensive emergency medicine billing services designed to support ED physicians, urgent care providers, trauma departments, and hospital-based emergency groups. Our team ensures accurate E/M level assignment, compliant documentation review, proper coding for critical care and procedures, and rapid claim submission — helping your emergency department achieve cleaner claims, fewer denials, and faster, more reliable reimbursements.
If your emergency medicine program needs a billing partner equipped to handle the pace and complexity of urgent, high-acuity care, MedVoice is here to strengthen your revenue cycle.
Proven Performance, Tangible Results
Our RCM workflows are built to support emergency departments dealing with acute, trauma, critical care, pediatric, and high-complexity encounters.
98%
Clean Claim Submission Rate
Every emergency medicine claim is reviewed for accuracy, completeness, and correct acuity-level coding.
40%
Reduction in A/R Days
Rapid submission + aggressive follow-up = significantly faster reimbursements.
99%
Coding Accuracy for Emergency Medicine
Our certified ED coders specialize in E/M levels, critical care, trauma billing, split/shared services, imaging, and procedures.
15%
Increase in Revenue Collection
Accurate documentation + compliant billing ensures predictable and consistent reimbursements.
Challenges We Solve for Emergency Medicine Practices
Emergency medicine billing is complex due to real-time documentation, multiple services in one encounter, and payer variations. MedVoice eliminates the issues that commonly drain ED revenue:
Incorrect E/M level assignment
Incomplete injury, accident, or work-comp documentation
Missing documentation for time-based critical care
Underbilling for procedures performed in the ED
Bundling errors for procedures & diagnostics
Misuse of modifier 25 for E/M + procedure
Denials for split/shared visits and scribe documentation
Delays due to high ED volume & rapid turnover
MedVoice ensures faster, cleaner, and compliant billing for all emergency encounters.
Why Emergency Medicine Billing Requires Specialized Expertise
Emergency departments run 24/7 and treat all acuity levels—from minor injuries to life-threatening conditions. Each encounter requires accurate coding that reflects complexity, time, and medical decision-making.
We specialize in:
- E/M coding for all ED levels (1–5)
- Critical care billing (time-based)
- Trauma & acute injury documentation
- Split/shared services for physicians & APPs
- Point-of-care ultrasound billing
- Diagnostic imaging & lab coding
- Minor & major ED procedures
- Motor vehicle accident & work-comp billing
- Pediatric emergency billing
- Observation services billing
- Scribe documentation compliance
MedVoice ensures accurate coding that protects your revenue and compliance.
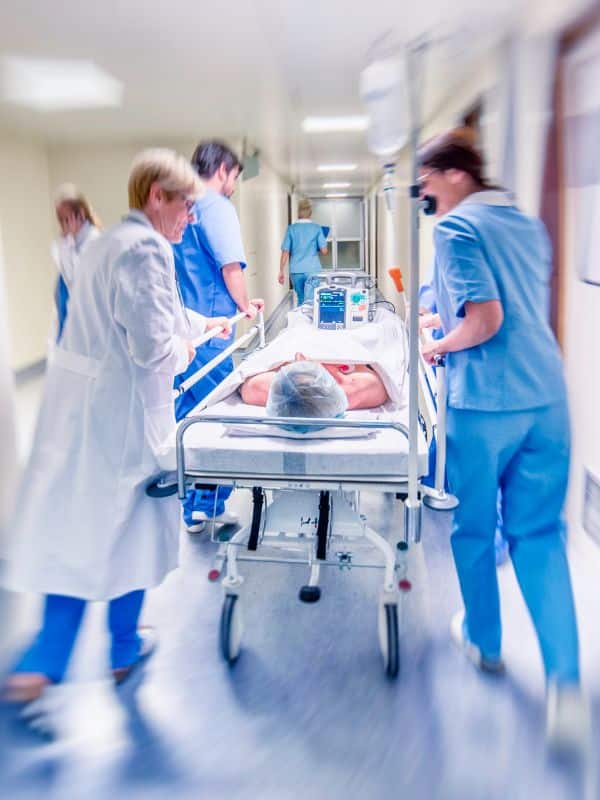
Why Choose MedVoice for Emergency Medicine Billing Services?
Some of The Common Emergency Medicine Diagnoses We Bill For (ICD-10 Codes)
We ensure precise ICD-10 coding for acute, trauma, and critical conditions.
- Chest pain — R07.9
- Abdominal pain — R10.9
- Shortness of breath — R06.02
- Fever — R50.9
- Acute injury/trauma — S00–T88 ranges
- Stroke symptoms — R29.810
- Hypertensive urgency — I16.0
- Sepsis — A41.9
- Dehydration — E86.0
- Syncope — R55
- Acute asthma exacerbation — J45.901
- COVID/viral illness — U07.1 / B34.9
We ensure all documentation supports medical necessity, session length, and treatment type to avoid payer rejections.
A Few Of The Emergency Medicine Procedures & Billing Codes We Support
Critical Care
- Initial critical care, 30–74 minutes — 99291
- Additional 30 minutes — 99292
Diagnostic & Imaging
- ECG interpretation — 93010
- X-ray interpretation — 71045–73590
- Ultrasound procedures — various CPTs
- CT/MRI interpretations (when applicable)
Respiratory & Cardiovascular
- Nebulizer treatment — 94640
- Non-invasive ventilation — 94660
- Cardioversion — 92960
Other Common ED Procedures
- Foreign body removal
- Incision & drainage — 10060
- IV infusion & hydration — 96360–96361
- Wound care and dressing changes
Who We Support
Our emergency medicine billing services support:
Emergency departments (ED)
Hospital emergency groups
Freestanding ERs
Urgent care centers
Trauma centers (Level I–III)
ED physician groups
Multi-specialty emergency care networks
Pediatric emergency departments
Compliance & Documentation Accuracy
Emergency medicine billing must meet strict CMS and payer-specific rules.
We ensure compliance with:
- E/M & critical care documentation standards
- Time-based billing guidelines
- Split/shared rules for ED providers
- Trauma and accident-specific documentation
- Correct CPT/ICD pairing
- Global period and bundling rules
- HIPAA, PHI, and emergency data security
Our billing audits help prevent payer audits and recoupments.
Benefits of Outsourcing to MedVoice
Outsourcing emergency medicine billing improves revenue flow and reduces claim backlogs—critical for high-volume ED operations.
- Higher reimbursement for E/M and critical care
- Reduced denials for imaging and trauma services
- Faster billing & payment cycles
- Lower administrative burden on ED staff
- Real-time financial reporting
- Lower cost versus in-house billing
- Emergency medicine–trained coders
- Scalable support for 24/7 ED operations
FAQ – Emergency Medicine Billing Services
Why is emergency medicine billing so complex?
Because ED services vary widely in acuity, require fast documentation, multiple procedures, and time-based coding.
Do you manage critical care billing?
Yes — including time audits, documentation checks, and accurate CPT application.
Do you support ED imaging & procedure billing?
Absolutely — including ECG, ultrasound, X-rays, laceration repairs, splints, and more.
How quickly do you submit ED claims?
Within 24–48 hours after receiving complete documentation.
Do you handle trauma, MVA, or worker’s comp billing?
Yes — including accident documentation and payer-specific requirements.
Request a FREE Emergency Medicine Billing Audit Today
Improve accuracy, reduce denials, and enhance emergency department revenue with MedVoice’s expert emergency medicine billing services. Our team ensures every ED encounter is coded correctly, documented fully, and reimbursed promptly.

