Outsource Medical Billing to the Experts.
Professional medical billing services for medical practices that improve collections, reduce denials, and streamline your revenue cycle.
MedVoice is a trusted name in medical billing outsourcing — helping physicians, hospitals, and clinics achieve accuracy, compliance, and efficiency. Our proven outsourced medical billing process ensures faster reimbursements, reduced denials, and complete transparency.
Partner with one of the leading medical billing outsourcing companies and focus more on patient care — while we handle your billing, coding, and revenue cycle.
98%
Clean Claim Rate
15%
Avg. Revenue Increase
40%
Reduction in A/R Days
Problems We Solve, So You Do Not Have To
Outsourcing your medical billing and coding to MedVoice helps eliminate the operational bottlenecks that slow down your revenue.
Claim Denials and Under Payments
Our predictive analytics ensure first pass resolution rates above 98%.
High Billing Costs
Reduced staffing, training, and operational expenses
Delayed reimbursements
Optimized follow-ups accelerated payments.
Limited Transparency
Gain complete visibility into your billing and collections with daily reporting and easy to understand dashboard.
Complex payer rules and compliance issues
Certified coders ensure accuracy across all payers and compliance officers ensure HIPAA and payer compliance.
Leakage & Write‑offs
Proactive audits to recover every payable dollar.
Customer Voice - In Their Own Words


Read More

AI + Human Expertise: The Future of Medical Billing Outsourcing







- Automated claim scrubbing & submission
- Real-time denial pattern analytics
- Revenue forecasting dashboards
- Fully HIPAA & SOC2 compliant infrastructure
- No hidden costs — No long-term contracts.
- Your revenue, fully optimized through intelligent automation.
The Way We Deliver Excellence
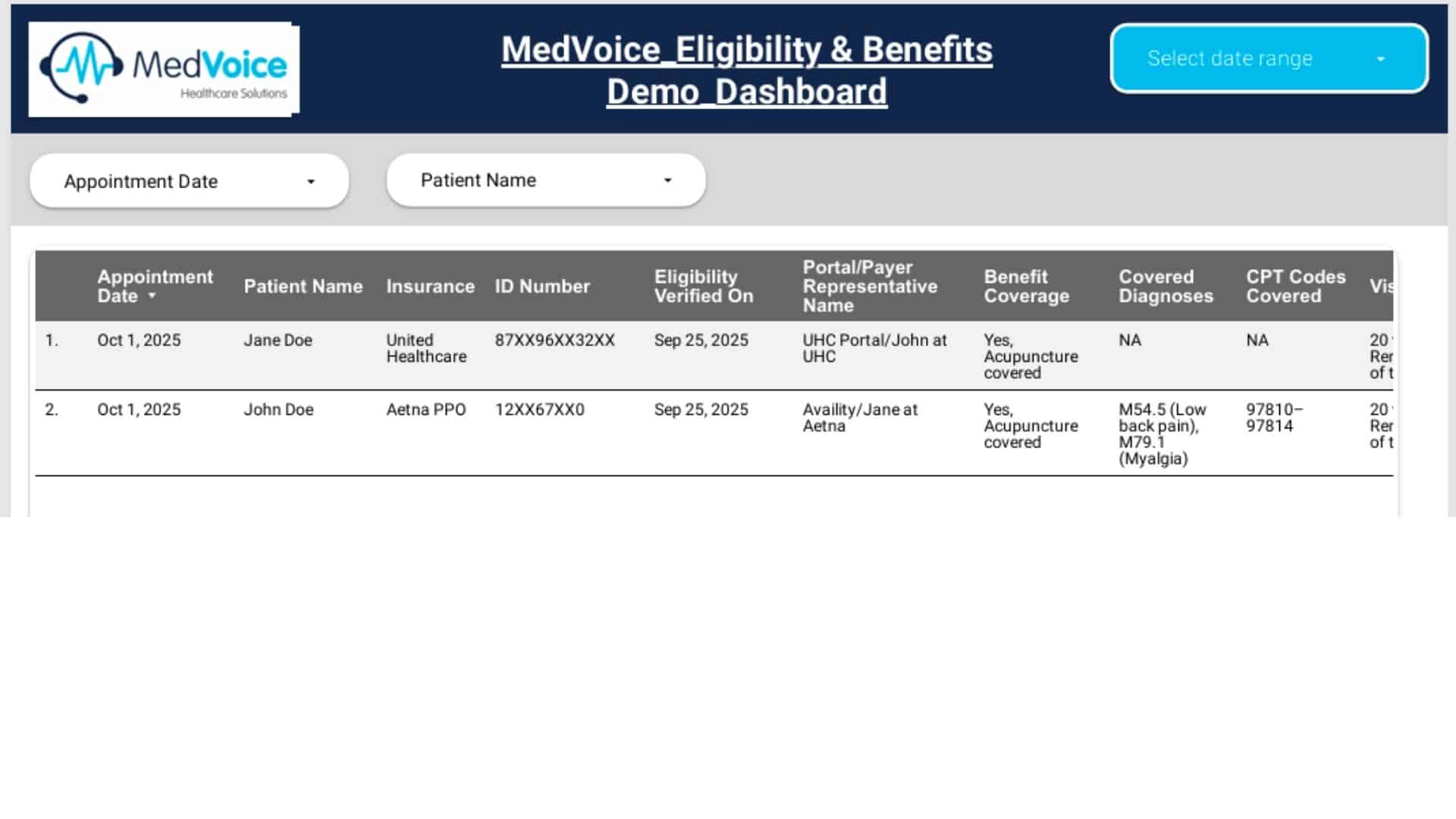
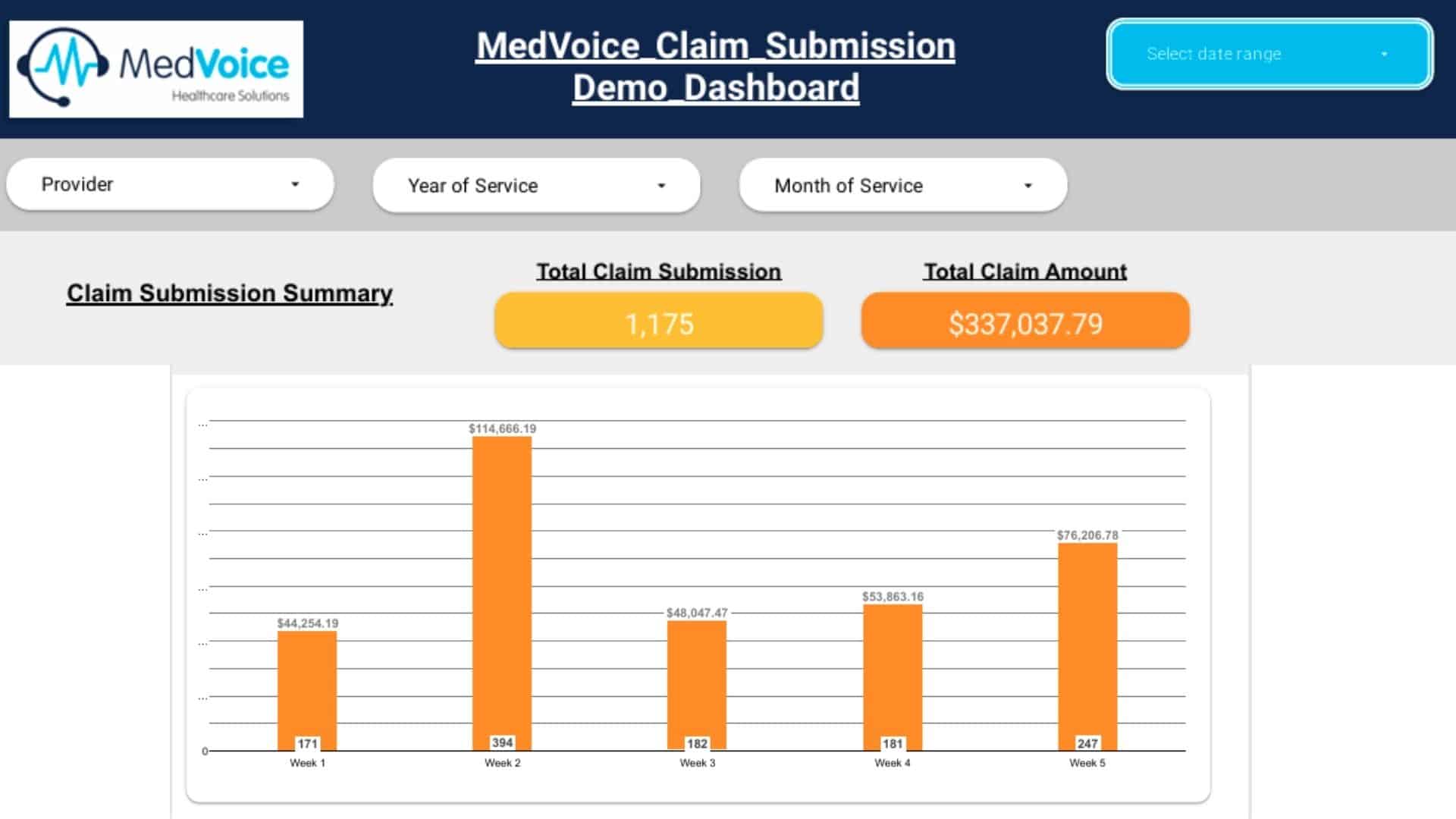
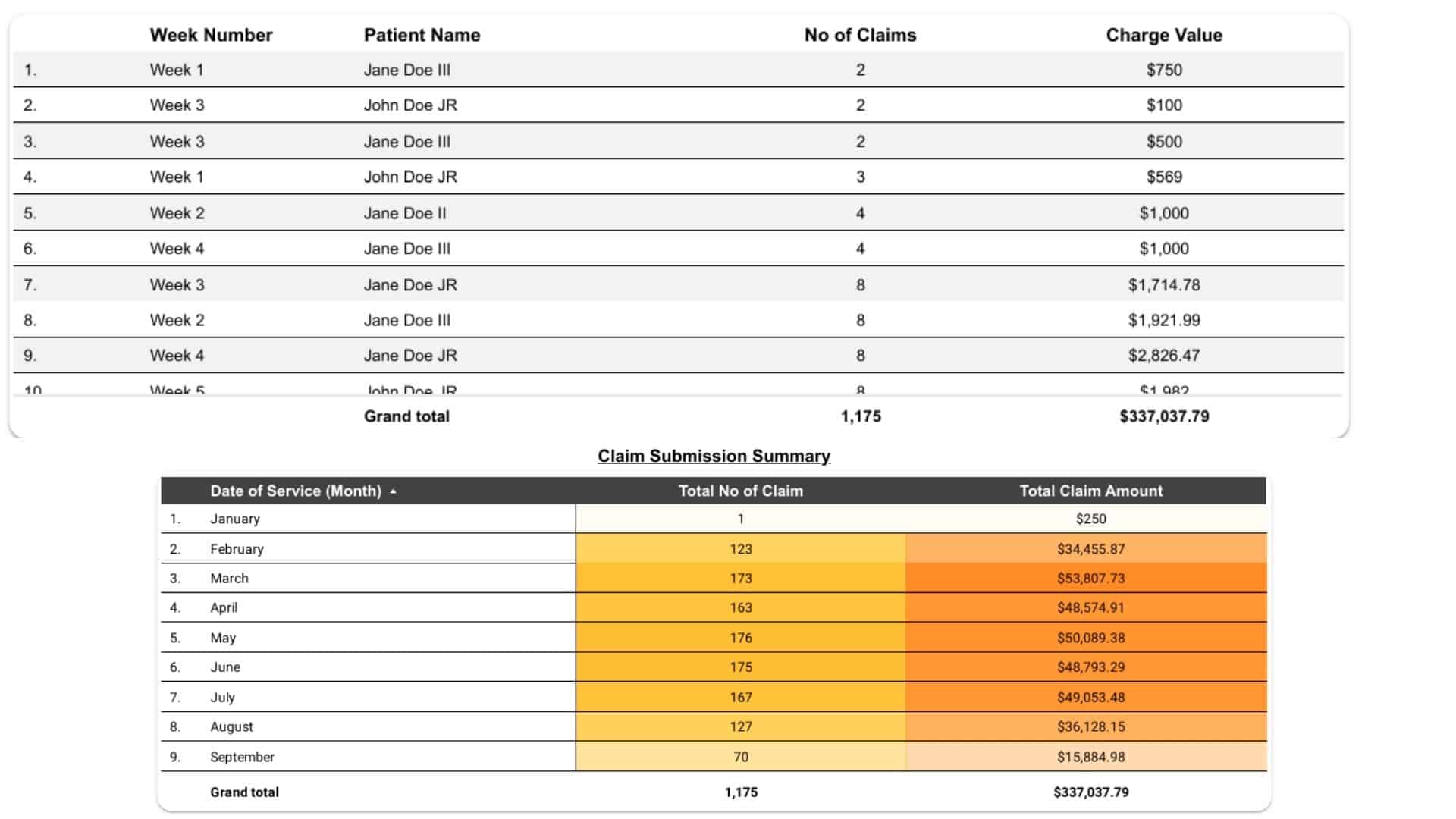
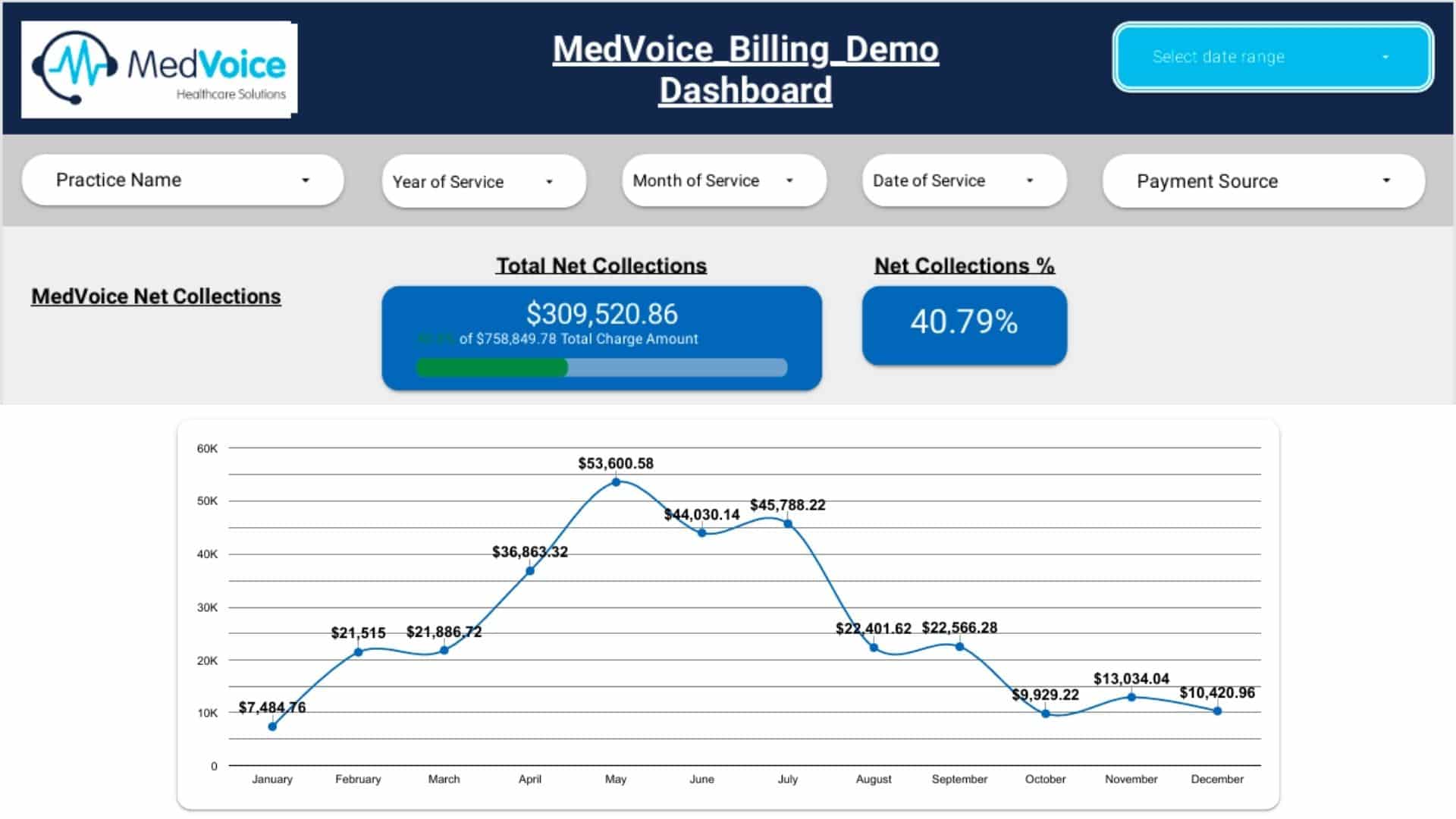
Practice Evaluation & Workflow Alignment
We start with a complete review of your specialty, patient volume, current billing system, and payer mix. Our team then designs a customized billing workflow that aligns with your existing EMR/EHR and coding guidelines — ensuring a smooth and seamless transition.
System Integration & Credentialing
We seamlessly integrate with your existing EHR, billing, and practice management systems to ensure uninterrupted workflows and secure data exchange. Our credentialing services manage provider enrollment, revalidation, and payer compliance, helping you go live faster and get paid without delays
Claims Submission & AR Management
We ensure every claim is accurately coded, verified, and submitted within 24 hours of documentation. Our dedicated AR specialists monitor each claim through its entire lifecycle, ensuring prompt payer responses and reducing days in A/R. With real-time tracking and denial alerts, we guarantee faster reimbursements and minimal revenue delays.
Intelligent Payment Posting & Reconciliation
Payments and EOBs/ERAs are posted with a blend of automated matching algorithms and manual oversight to ensure accuracy and prevent revenue leakage. Any discrepancies are flagged instantly for correction.
Payment Posting & Denial Resolution
Our RCM team performs precise payment posting with automated EOB/ERA matching and reconciliation. Any underpayments or rejections trigger instant alerts for investigation. Denials are analyzed at the root-cause level, corrected, and resubmitted promptly—ensuring maximum revenue recovery and zero revenue leakage.
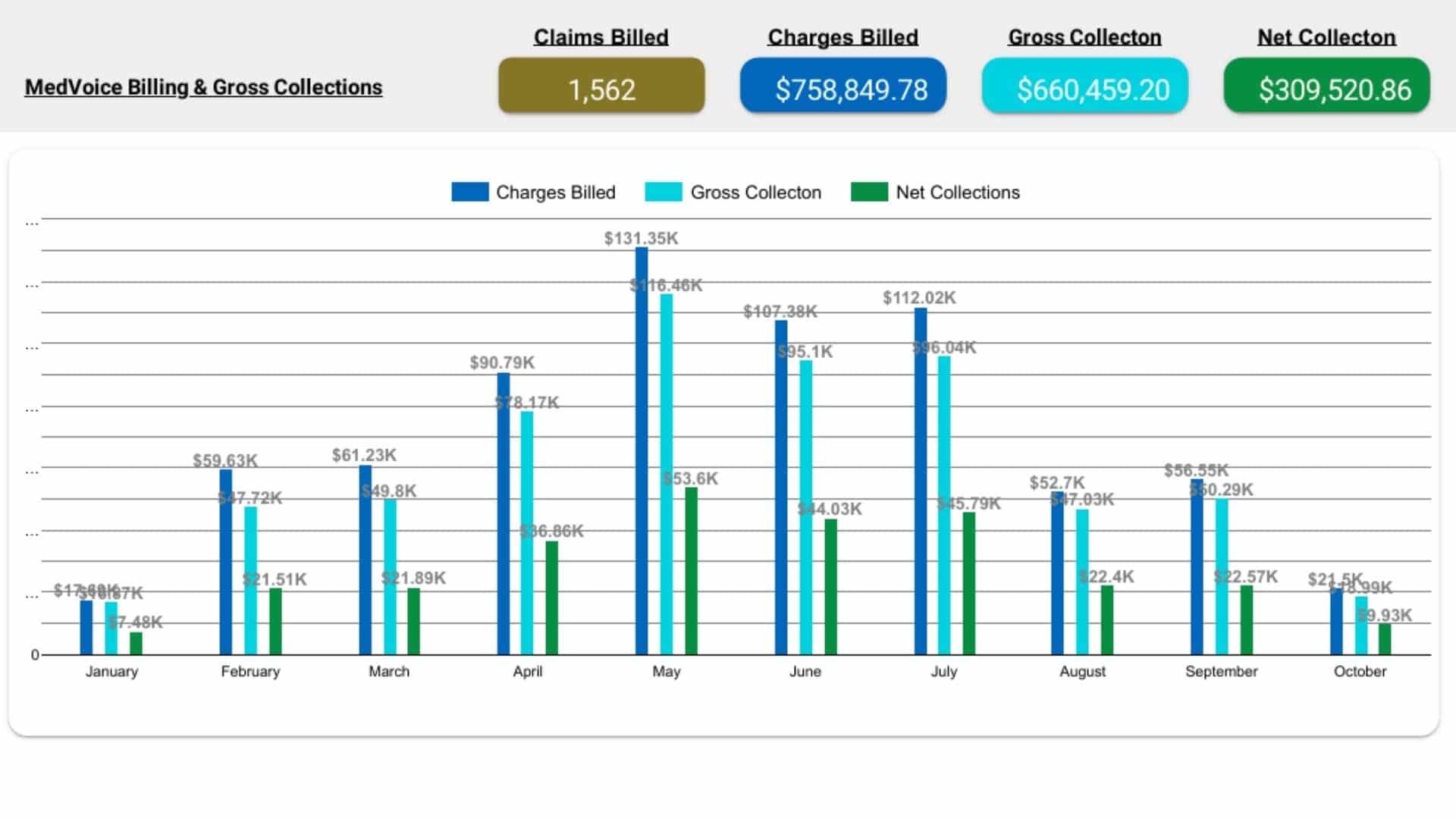
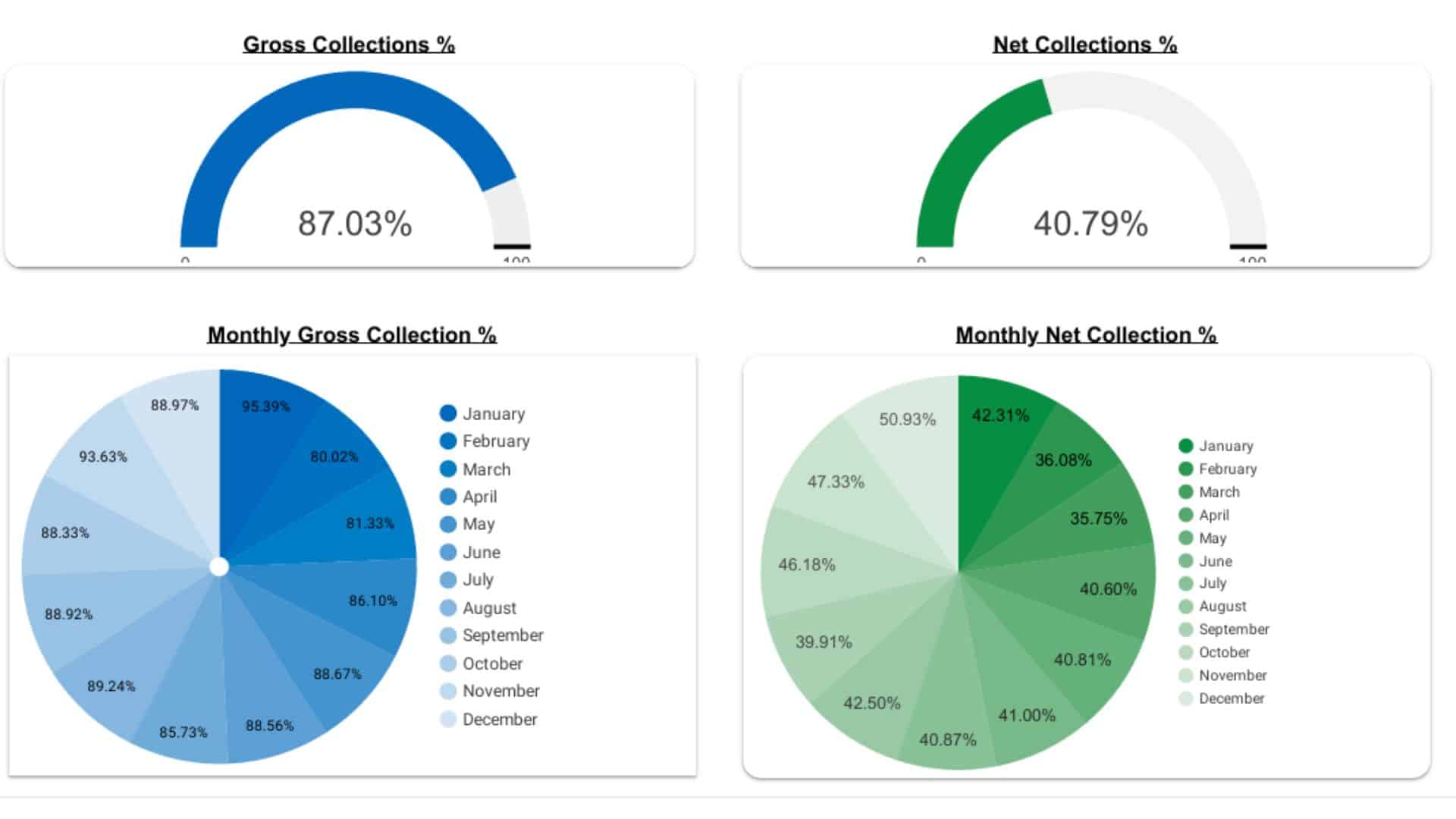
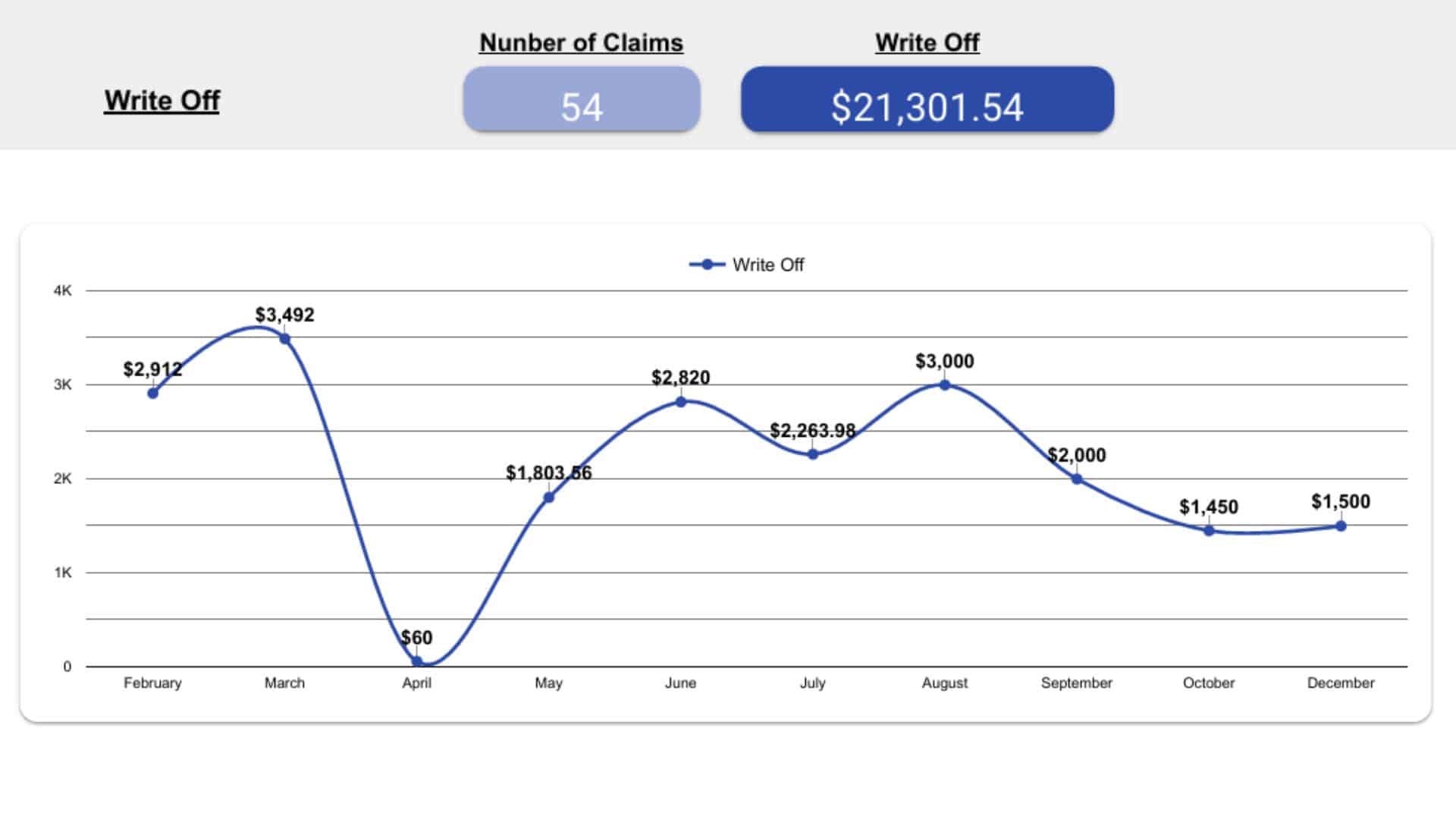
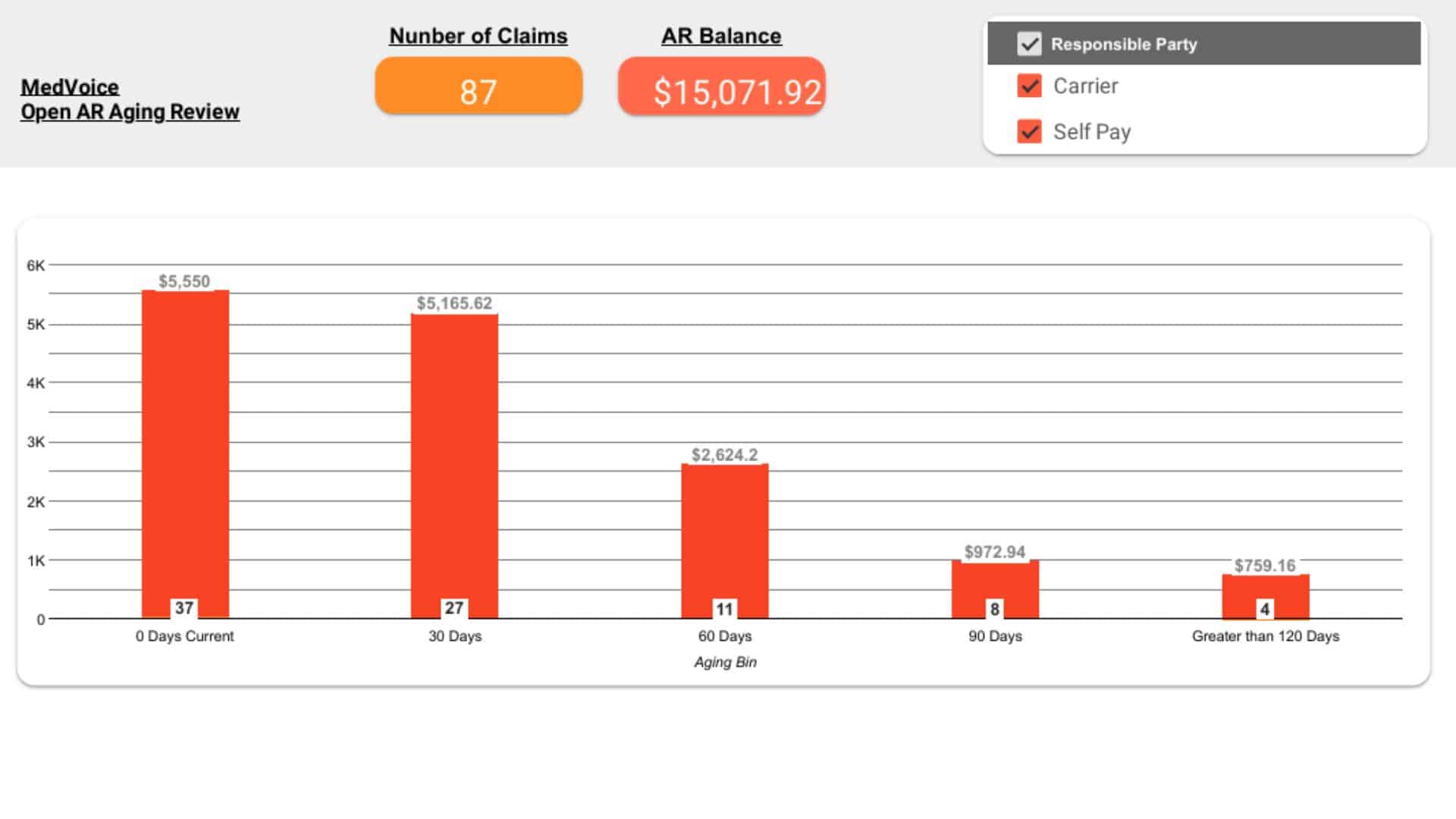
Performance Reports & Optimization
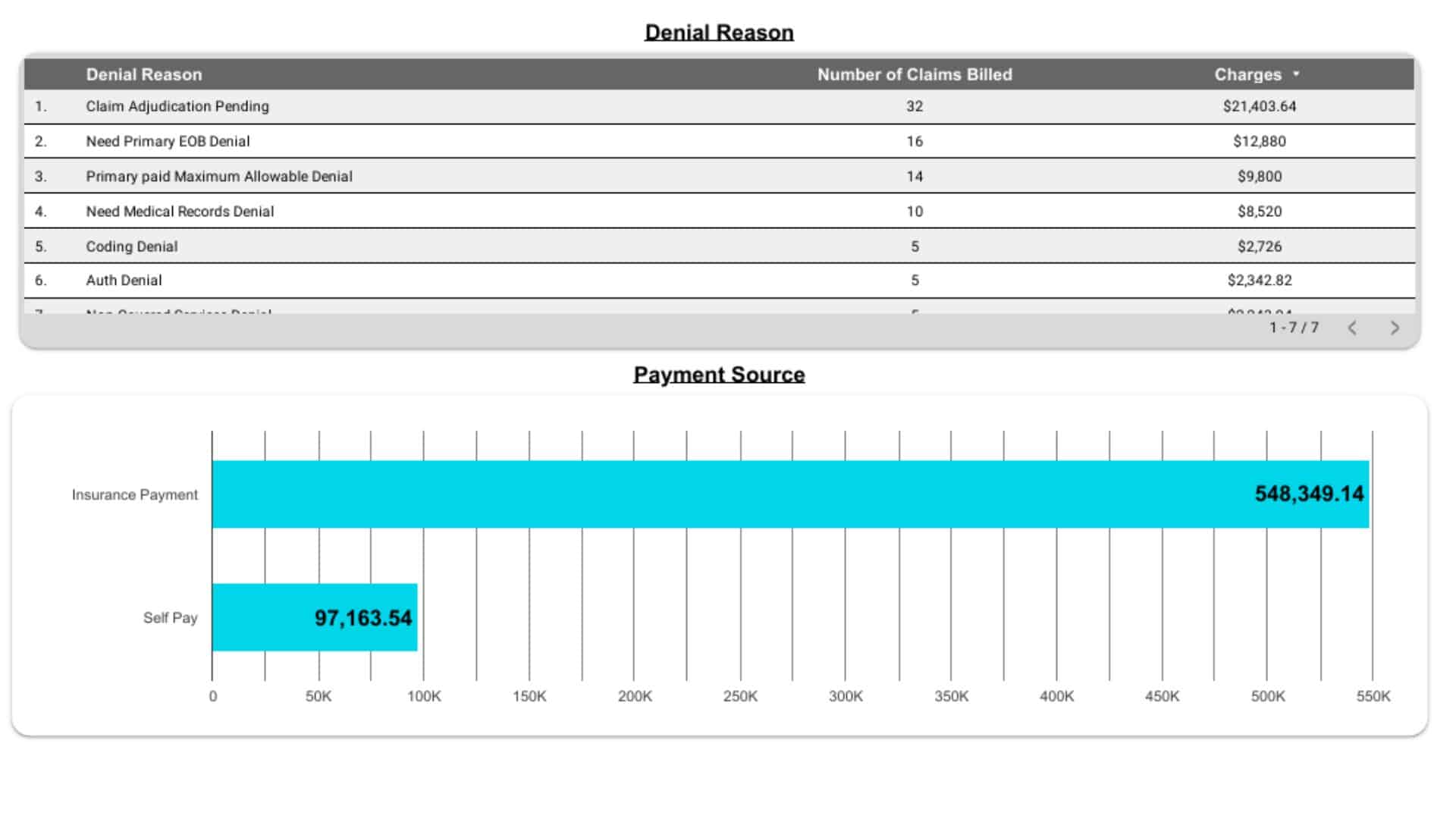
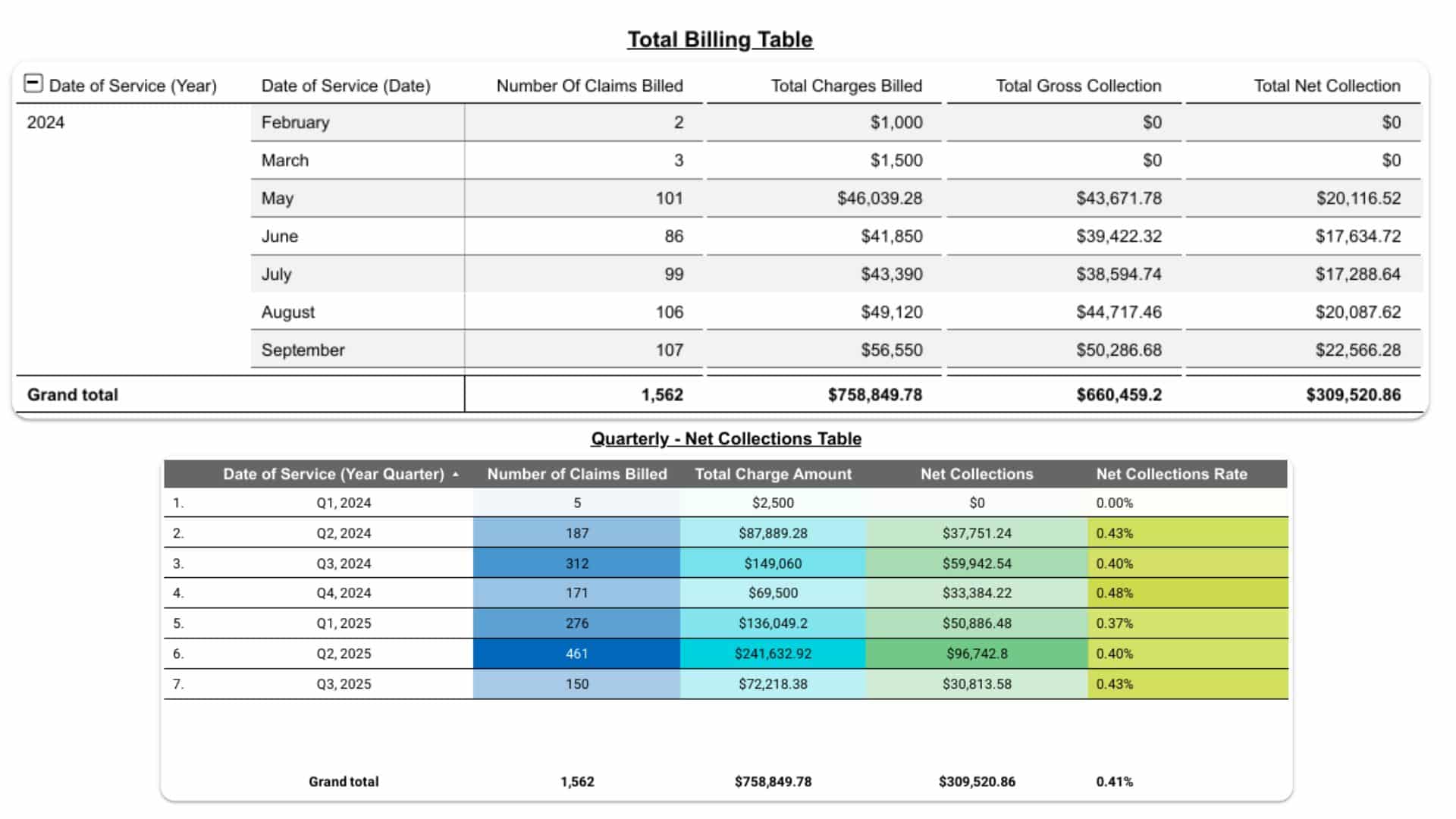
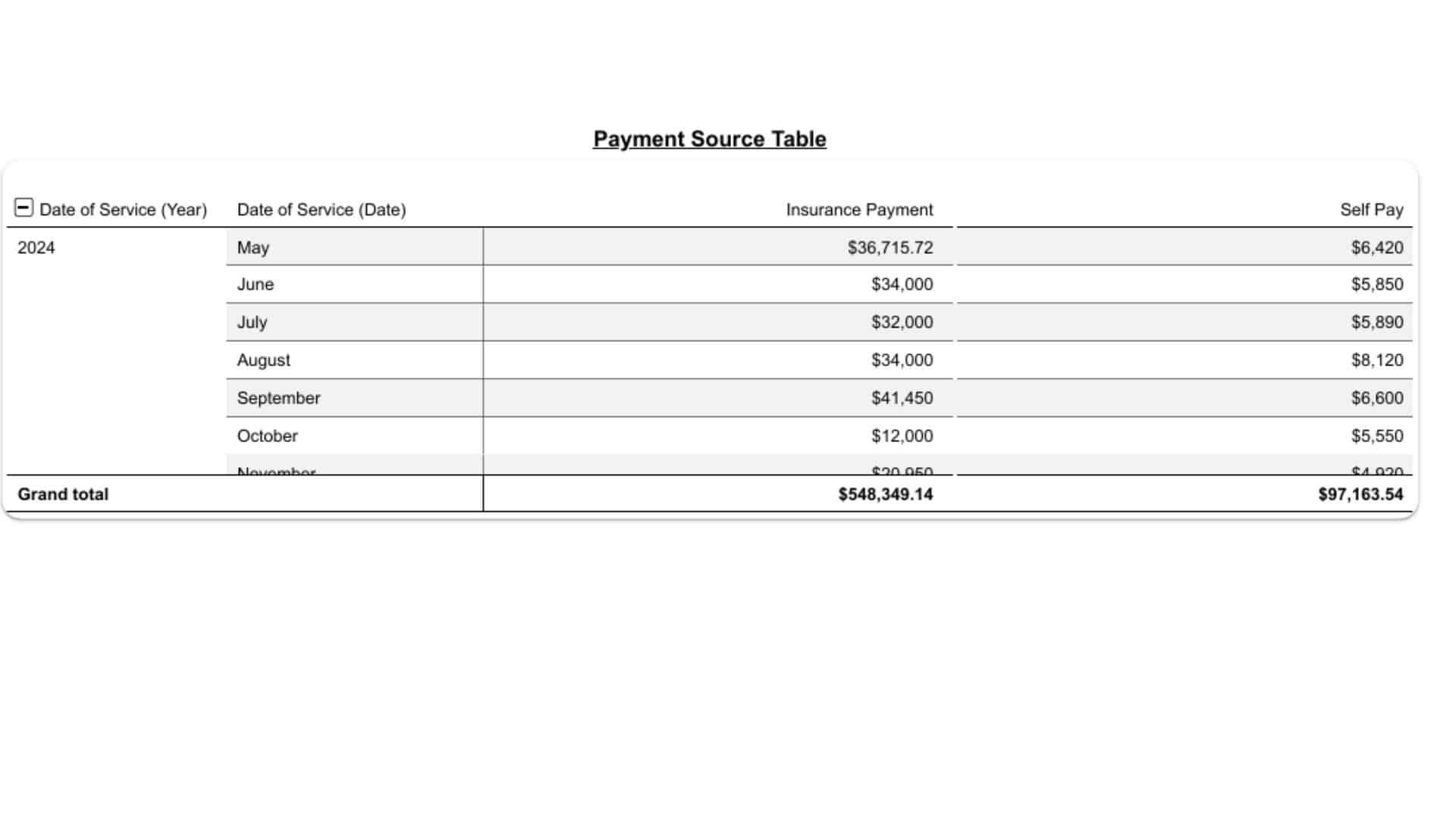
We provide transparent, data-driven performance dashboards that highlight every key metric—collections, denials, AR aging, and payer trends. Monthly performance reviews and revenue insights help optimize workflows, strengthen compliance, and identify growth opportunities for your practice.
Practice Evaluation & Workflow Alignment
We start with a complete review of your specialty, patient volume, current billing system, and payer mix. Our team then designs a customized billing workflow that aligns with your existing EMR/EHR and coding guidelines — ensuring a smooth and seamless transition.
System Integration & Credentialing
We seamlessly integrate with your existing EHR, billing, and practice management systems to ensure uninterrupted workflows and secure data exchange. Our credentialing services manage provider enrollment, revalidation, and payer compliance, helping you go live faster and get paid without delays
Claims Submission & AR Management
We ensure every claim is accurately coded, verified, and submitted within 24 hours of documentation. Our dedicated AR specialists monitor each claim through its entire lifecycle, ensuring prompt payer responses and reducing days in A/R. With real-time tracking and denial alerts, we guarantee faster reimbursements and minimal revenue delays.
Intelligent Payment Posting & Reconciliation
Payments and EOBs/ERAs are posted with a blend of automated matching algorithms and manual oversight to ensure accuracy and prevent revenue leakage. Any discrepancies are flagged instantly for correction.
Payment Posting & Denial Resolution
Our RCM team performs precise payment posting with automated EOB/ERA matching and reconciliation. Any underpayments or rejections trigger instant alerts for investigation. Denials are analyzed at the root-cause level, corrected, and resubmitted promptly—ensuring maximum revenue recovery and zero revenue leakage.
Performance Reports & Optimization
We provide transparent, data-driven performance dashboards that highlight every key metric—collections, denials, AR aging, and payer trends. Monthly performance reviews and revenue insights help optimize workflows, strengthen compliance, and identify growth opportunities for your practice.
Our Areas of Excellence
Primary Care & Internal Medicine
Outsource primary care billing for faster reimbursements and error-free claims.
Cardiology & Orthopedics
Specialized outsourcing for cardiology and orthopedic billing to reduce denials and improve cash flow.
Behavioral Health & Psychiatry:
Outsource mental health billing for clean claims, compliance, and higher collections.
Anesthesiology & Pain Management
Pain-free outsourcing for anesthesia billing—accurate coding and faster payments.
Urgent Care & Home Health
Streamline urgent care and home health billing with outsourced experts for maximum efficiency.
Flexible Medical Billing Pricing
- Percentage of collections
- Customized pricing for high-volume practices


Frequently Asked Questions
What are your fees?
How do you ensure data security?
What specialties do you work with?
How long does it take to get started?
Ready to eliminate billing headaches and boost your reimbursements?

Services
- Medical Billing
- AI Medical Scribing
- Claims Management
- Revenue Cycle Management
AI Tools
- AI Scribe
- AI Coding Assistant
- Documentation Tools
- Compliance Monitor

