Smarter Medical Billing - Greater Savings. Maximized Revenue.
98%
Clean Claim Rate
15%
Avg. Revenue Increase
40%
Reduction in A/R Days
Problems We Solve
High Denial Rates
Automated edits and audits reduce rework.
Limited Visibility
Real-time dashboards improve decision-making.
Slow Reimbursements
Optimized follow-ups accelerated payments.
Multi‑Specialty Complexity
Tailored workflows for every specialty.
Compliance & Coding Gaps
Certified coders ensure HIPAA and payer compliance.
Leakage & Write‑offs
Proactive audits to recover every payable dollar.
The Complete Medical Billing Solution for Modern Healthcare Professionals
Customer Voice - In Their Own Words


Read More

AI Technology – Included at No Extra Cost







- Real-Time AI-Powered Documentation
- Intelligent Coding Assistance
- Higher Clean Claim Rates
- Reduced A/R Days
- Faster Revenue Cycle
- Increased Practice Revenue
- No Extra Cost. Fully Bundled.
- Less Admin. More Focus on Care.
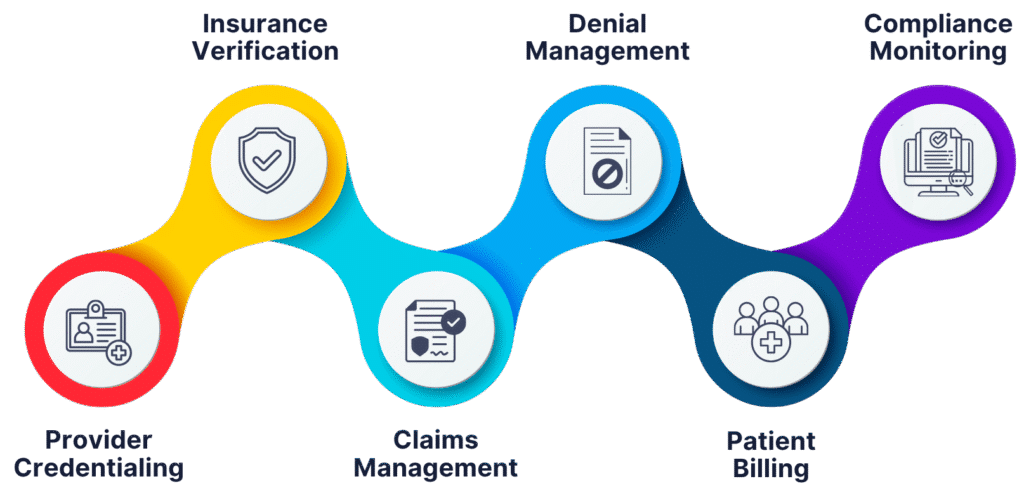
The Way We Deliver Excellence
Practice Evaluation & Workflow Alignment
We start with a complete review of your specialty, patient volume, current billing system, and payer mix. Our team then designs a customized billing workflow that aligns with your existing EMR/EHR and coding guidelines — ensuring a smooth and seamless transition.
AI-Assisted Coding with Human Verification
Our platform leverages AI-powered code prediction and documentation analysis to identify the most accurate medical codes. Every code is then verified by certified AAPC/AHIMA coders to ensure compliance, specialty accuracy, and optimal reimbursement — eliminating under-coding and over-coding risks.
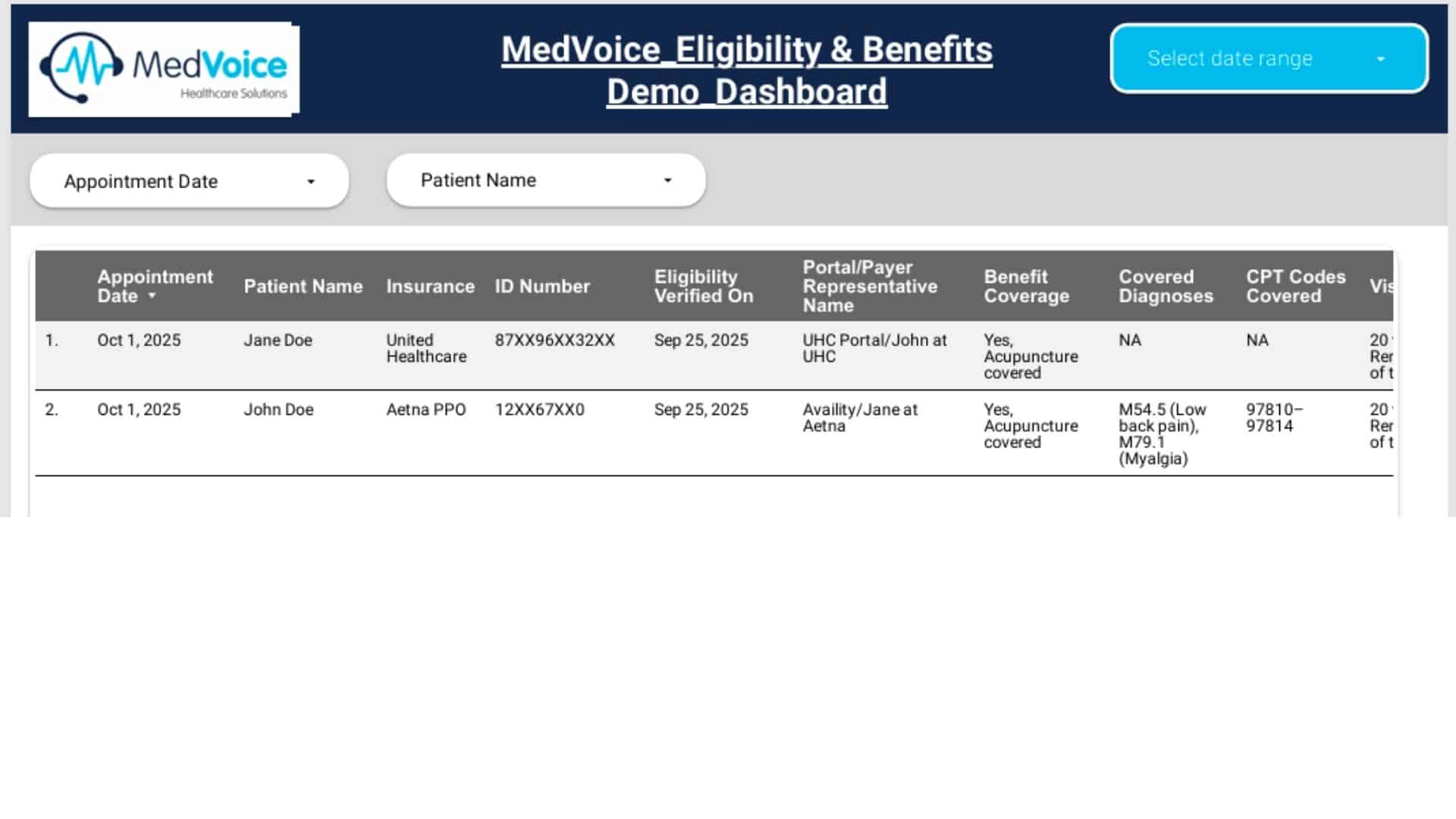
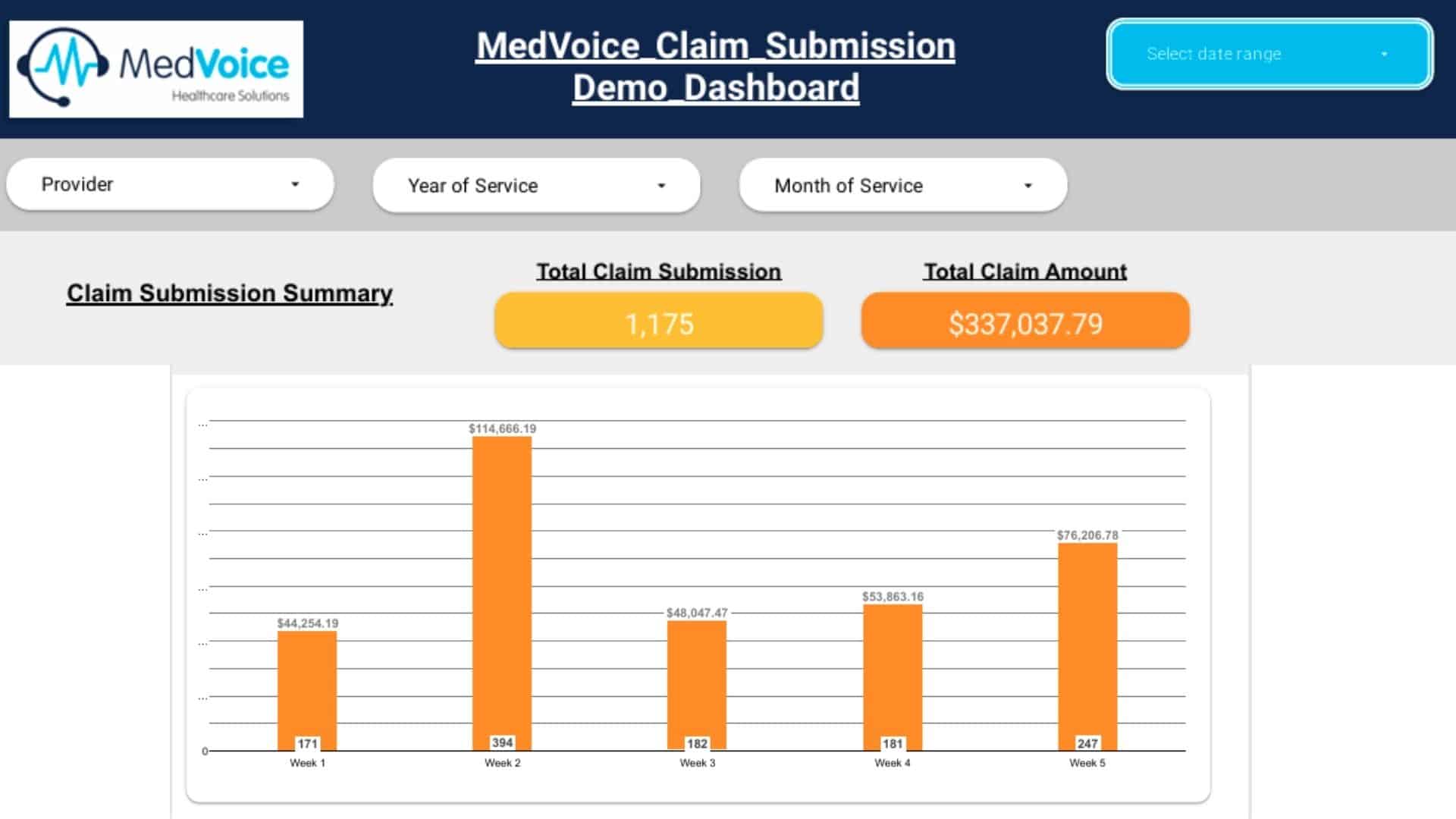
Clean Claim Preparation & Submission
Claims are automatically screened using AI-driven claim scrubbing tools to flag errors before submission. Our billing specialists then perform final compliance checks to ensure payer readiness — helping achieve first-pass claim acceptance.
Intelligent Payment Posting & Reconciliation
Payments and EOBs/ERAs are posted with a blend of automated matching algorithms and manual oversight to ensure accuracy and prevent revenue leakage. Any discrepancies are flagged instantly for correction.
Proactive Denial Analytics & Resolution
Our AI tools continuously monitor denials to identify patterns and root causes. Our RCM experts then act quickly to correct, appeal, and resubmit claims — improving recovery rates and reducing recurring denials.
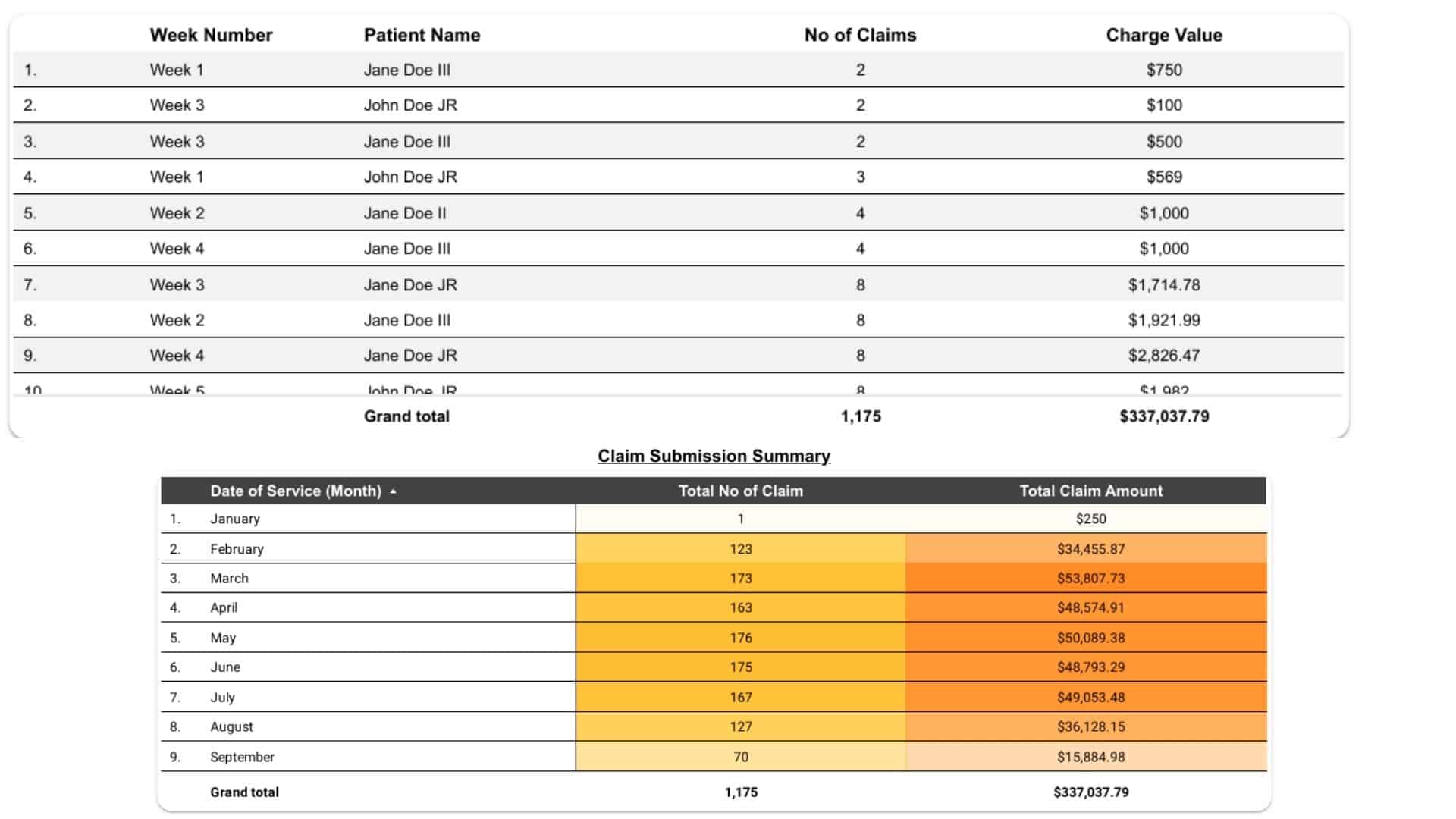
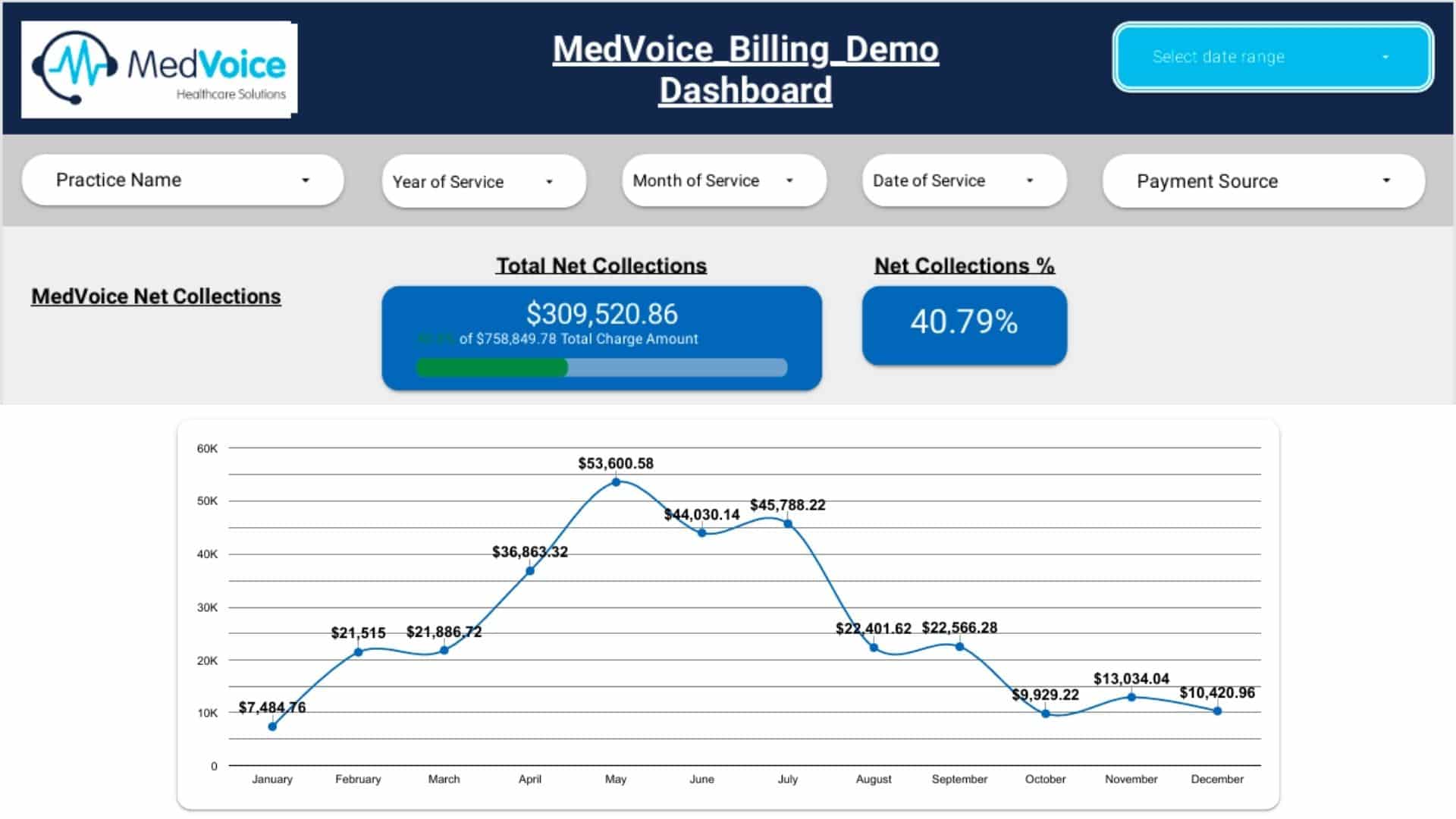
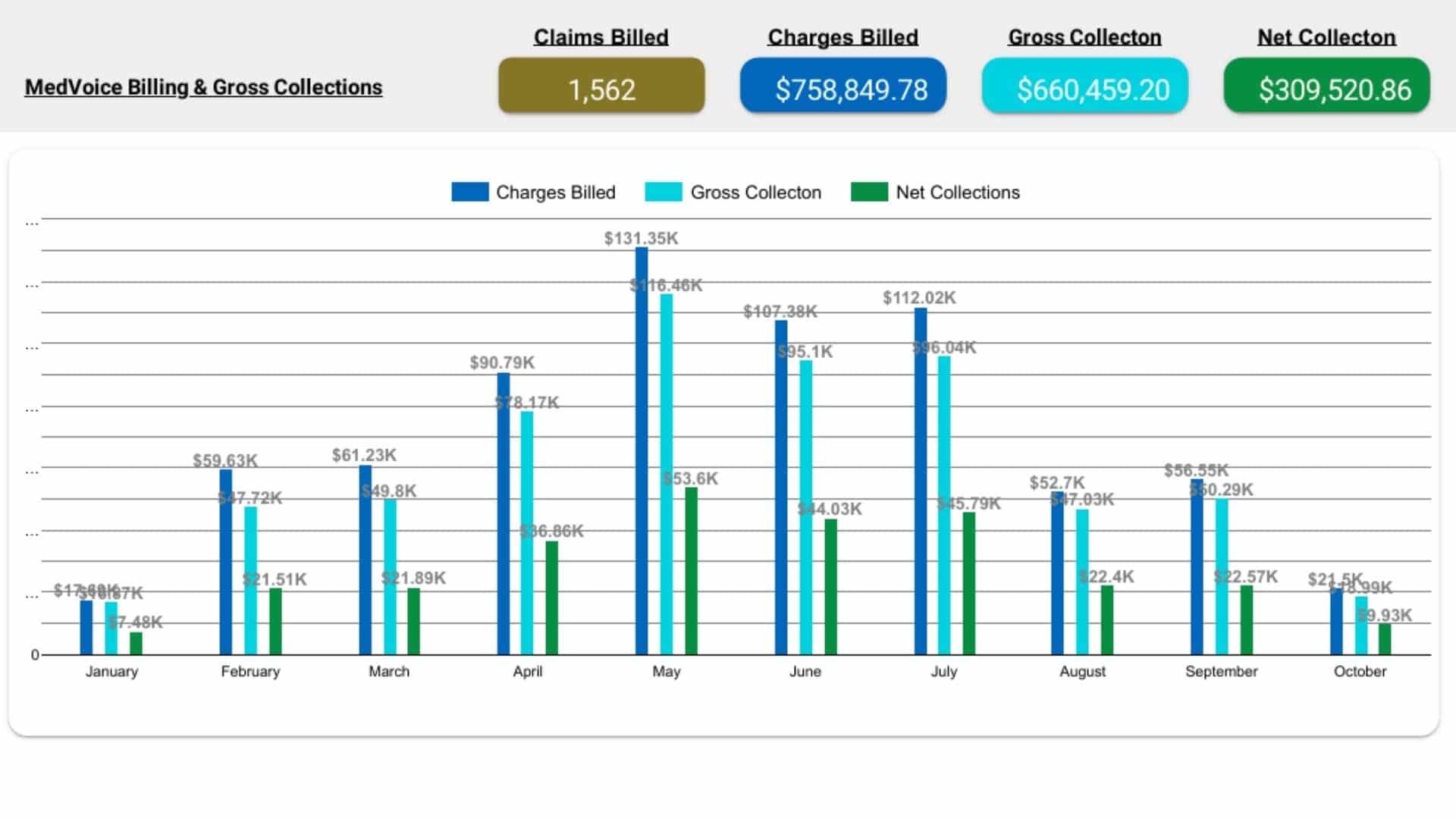
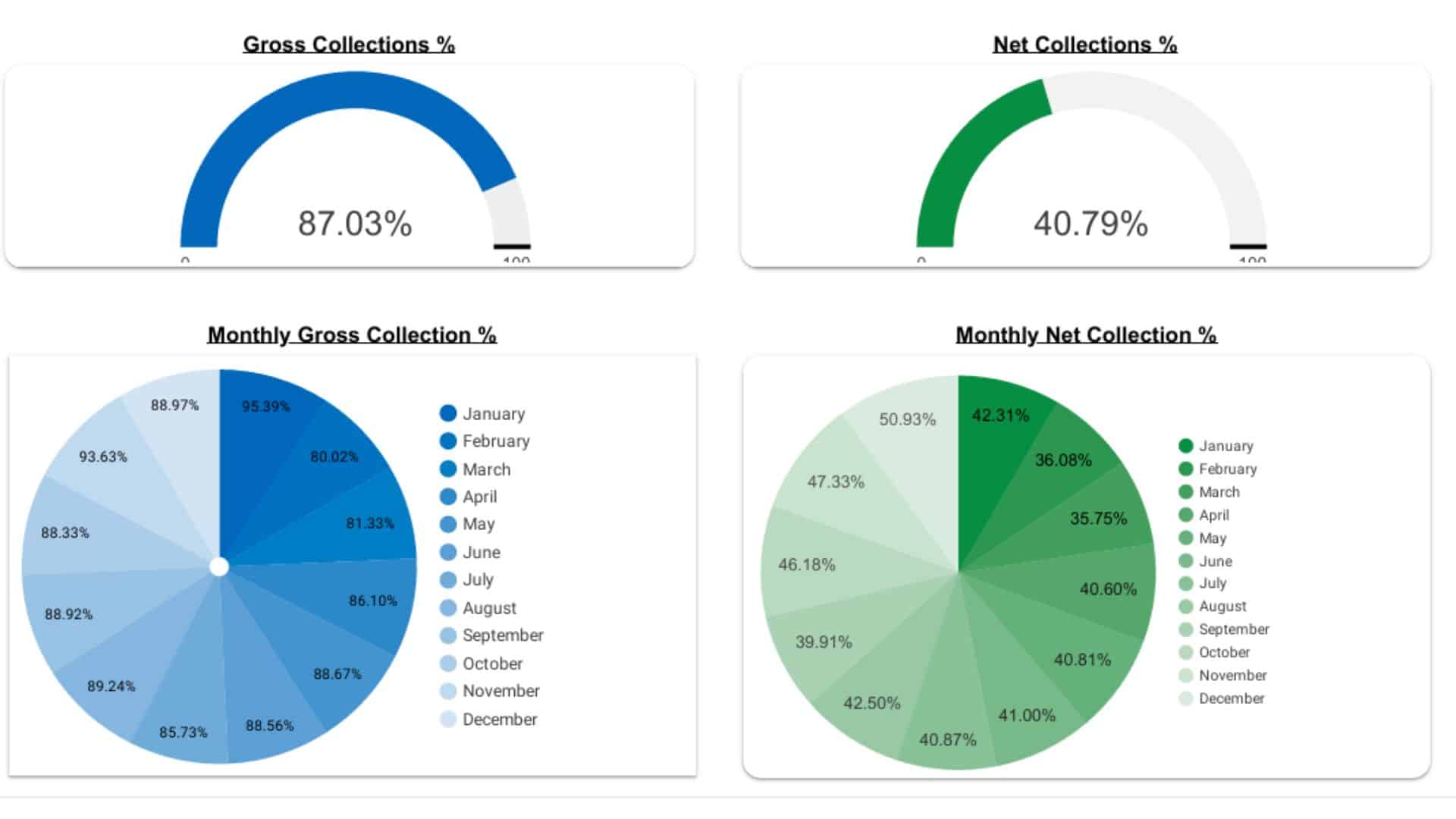
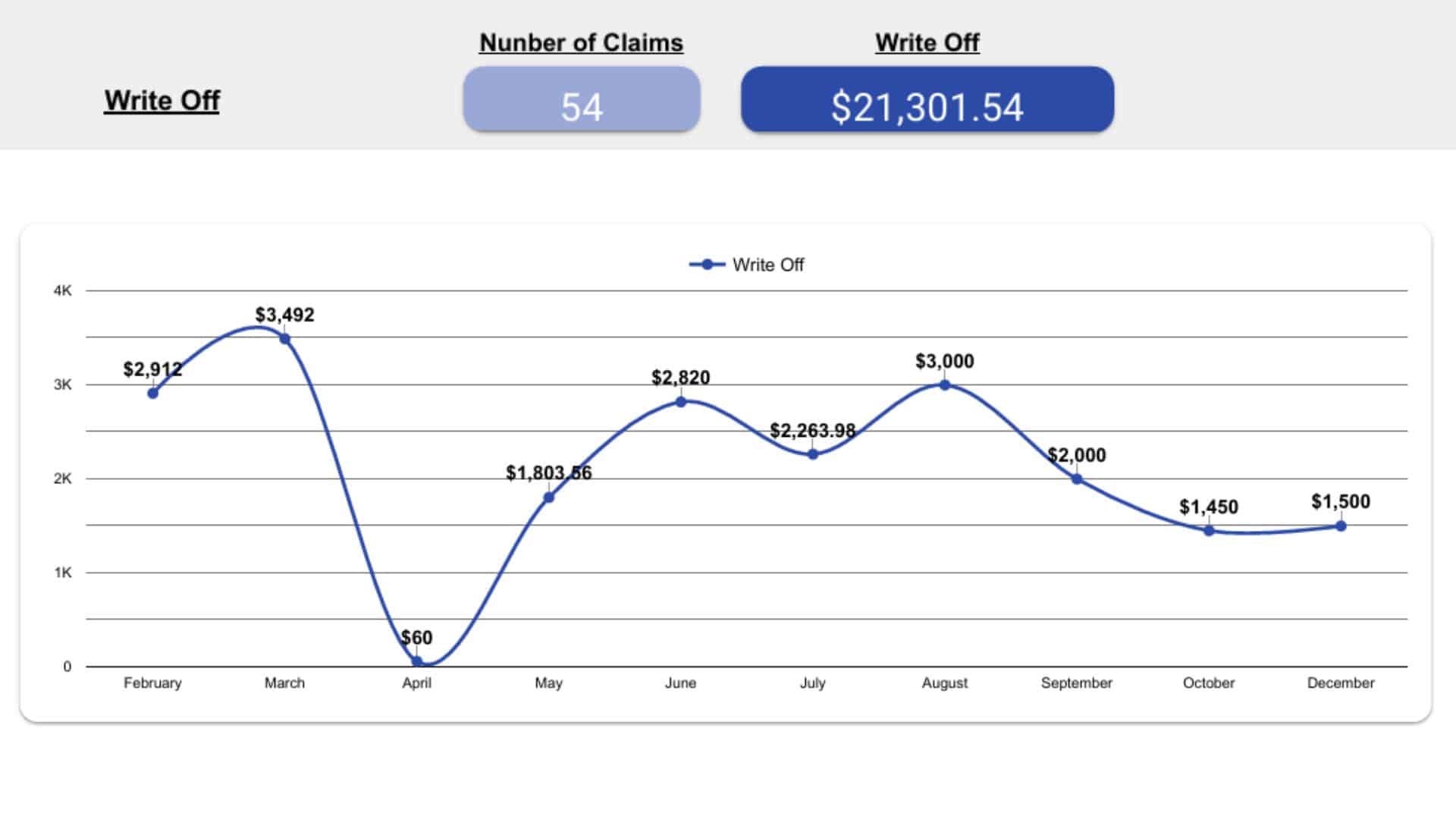
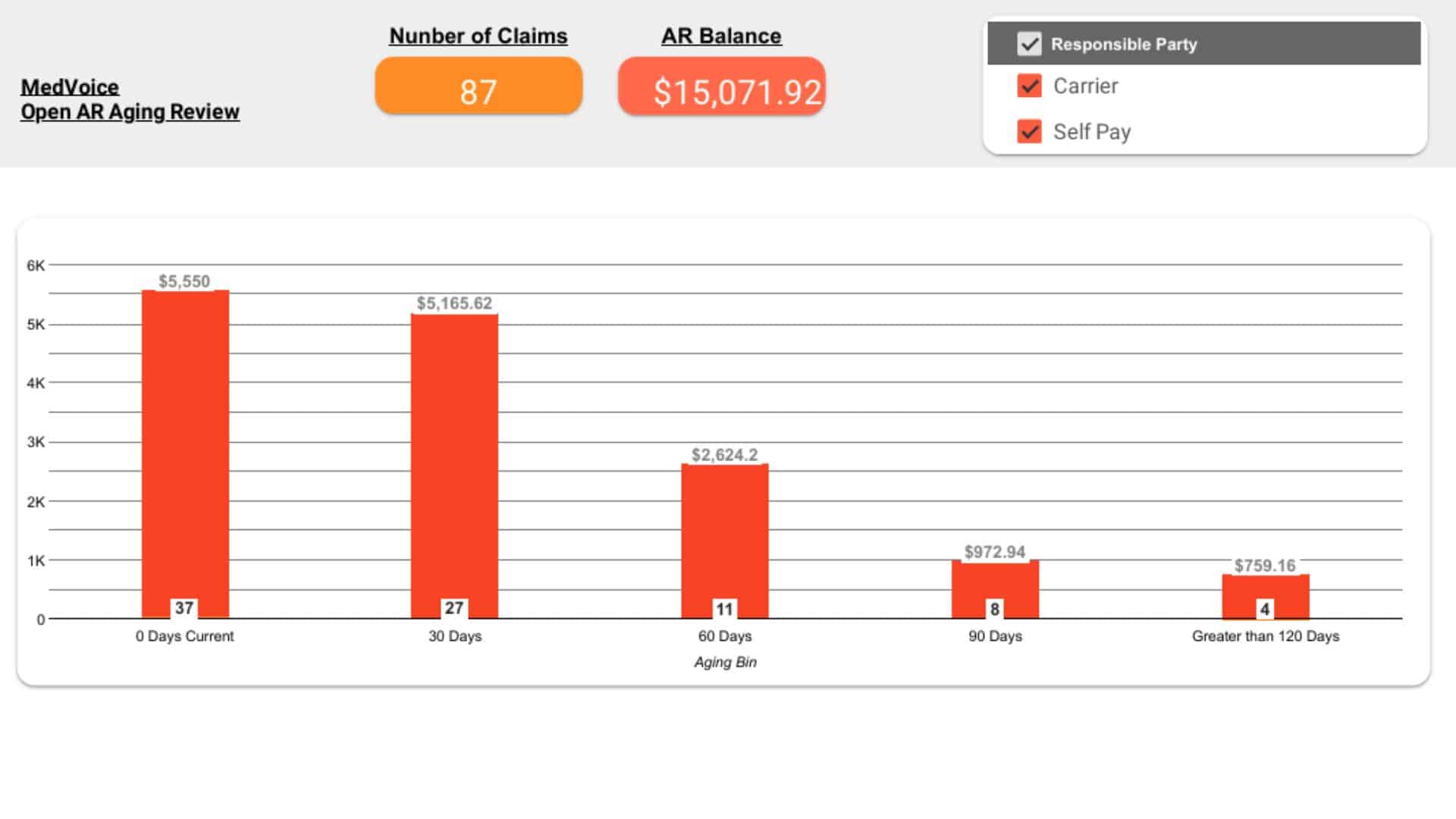
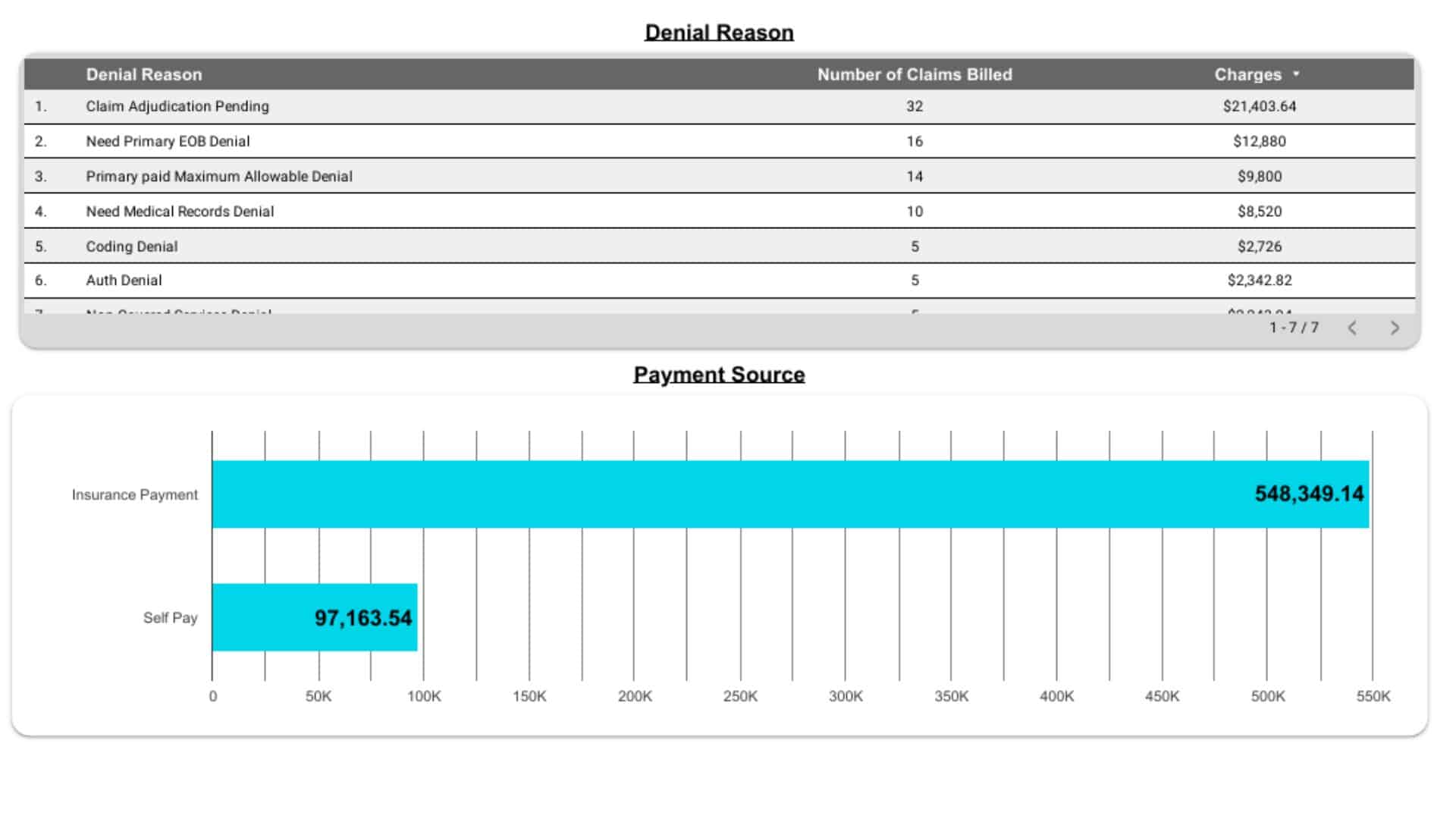
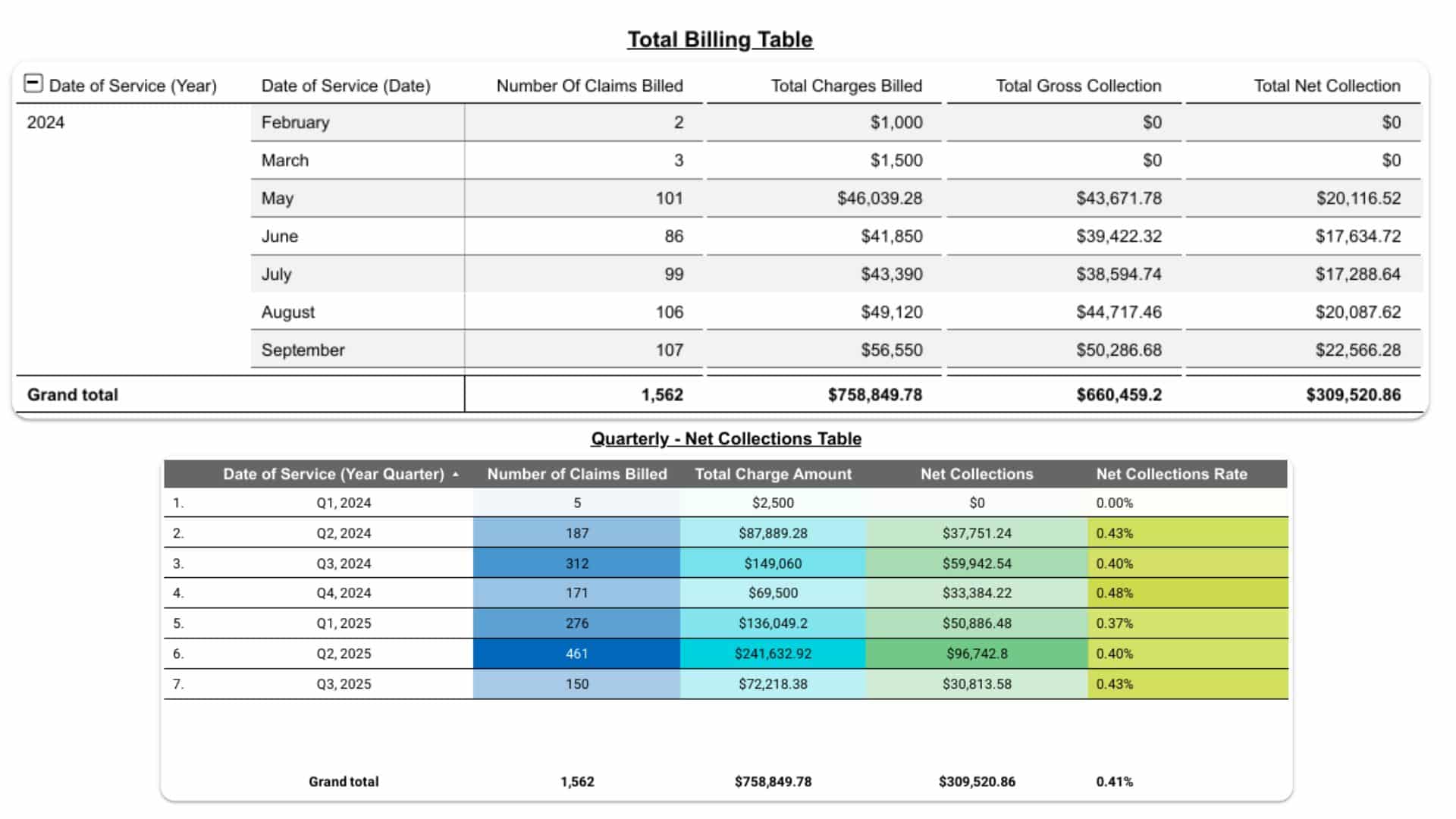
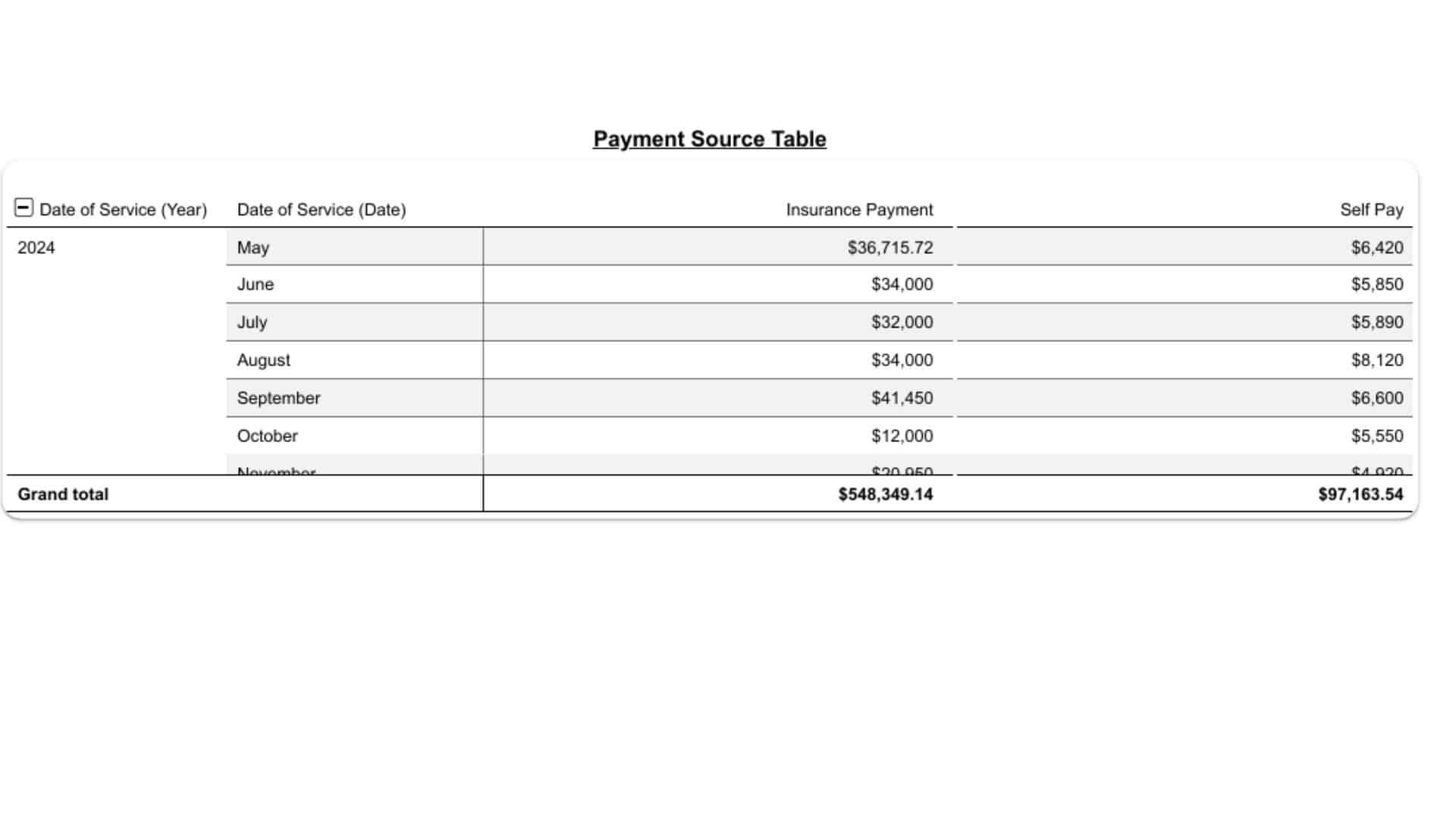
Performance Reporting & Revenue Insights
You receive transparent, data-driven reports with:
- Collection efficiency
- Denial trend analysis
- Payer performance comparison
- Financial KPIs and revenue forecasts
Practice Evaluation & Workflow Alignment
We start with a complete review of your specialty, patient volume, current billing system, and payer mix. Our team then designs a customized billing workflow that aligns with your existing EMR/EHR and coding guidelines — ensuring a smooth and seamless transition.
AI-Assisted Coding with Human Verification
Our platform leverages AI-powered code prediction and documentation analysis to identify the most accurate medical codes. Every code is then verified by certified AAPC/AHIMA coders to ensure compliance, specialty accuracy, and optimal reimbursement — eliminating under-coding and over-coding risks.
Clean Claim Preparation & Submission
Claims are automatically screened using AI-driven claim scrubbing tools to flag errors before submission. Our billing specialists then perform final compliance checks to ensure payer readiness — helping achieve first-pass claim acceptance.
Intelligent Payment Posting & Reconciliation
Payments and EOBs/ERAs are posted with a blend of automated matching algorithms and manual oversight to ensure accuracy and prevent revenue leakage. Any discrepancies are flagged instantly for correction.
Proactive Denial Analytics & Resolution
Our AI tools continuously monitor denials to identify patterns and root causes. Our RCM experts then act quickly to correct, appeal, and resubmit claims — improving recovery rates and reducing recurring denials.
Performance Reporting & Revenue Insights
You receive transparent, data-driven reports with:
- Collection efficiency
- Denial trend analysis
- Payer performance comparison
- Financial KPIs and revenue forecasts
Our Footprints
Why Choose MedVoice Medical Billing Services in California?
California’s vast and complex healthcare landscape, with its diverse patient populations, intricate regulatory frameworks, and numerous payer systems, demands a highly sophisticated approach to medical billing. MedVoice possesses an in-depth understanding of the specific payer requirements and state-level regulations prevalent in California, ensuring not only accurate billing but also unwavering compliance. Our advanced AI-driven tools, combined with the expertise of our dedicated team, empower healthcare practices across California to achieve tangible results, including:
Why Texas Practices Choose Our Medical Billing Solutions
Texas’s vast and diverse healthcare landscape, with its major metropolitan areas, sprawling rural regions, and specific state regulations, requires a robust and adaptable approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Texas, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Texas achieve:
Why Choose MedVoice in Florida?
Florida’s dynamic healthcare landscape, with its large and diverse population, numerous medical facilities, and specific state regulations, requires a robust approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Florida, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Florida achieve:
Why Choose MedVoice in New York?
New York’s complex healthcare landscape, with its vast urban centers, diverse patient populations, and intricate state regulations, requires a highly specialized approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within New York, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in New York achieve:
Why Choose MedVoice in Pennsylvania?
Pennsylvania’s diverse healthcare landscape, with its major urban centers and rural areas, along with specific state regulations, requires a robust approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Pennsylvania, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Pennsylvania achieve:
Alabama
Alaska
Arizona
Arkansas
California
Colorado
Connecticut
Delaware
Florida
Georgia
Hawaii
Idaho
Illinois
Indiana
Iowa
Kansas
Kentucky
Louisiana
Maine
Maryland
New Mexico
New York
North Carolina
North Dakota
Ohio
Oklahoma
Oregon
Pennsylvania
Rhode Island
South Carolina
South Dakota
Tennessee
Texas
Utah
Vermont
Virginia
Washington
West Virginia
Wisconsin
Wyoming
California
Why Choose MedVoice Medical Billing Services in California?
California’s vast and complex healthcare landscape, with its diverse patient populations, intricate regulatory frameworks, and numerous payer systems, demands a highly sophisticated approach to medical billing. MedVoice possesses an in-depth understanding of the specific payer requirements and state-level regulations prevalent in California, ensuring not only accurate billing but also unwavering compliance. Our advanced AI-driven tools, combined with the expertise of our dedicated team, empower healthcare practices across California to achieve tangible results, including:
Texas
Why Texas Practices Choose Our Medical Billing Solutions
Texas’s vast and diverse healthcare landscape, with its major metropolitan areas, sprawling rural regions, and specific state regulations, requires a robust and adaptable approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Texas, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Texas achieve:
Florida
Why Choose MedVoice in Florida?
Florida’s dynamic healthcare landscape, with its large and diverse population, numerous medical facilities, and specific state regulations, requires a robust approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Florida, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Florida achieve:
New York
Why Choose MedVoice in New York?
New York’s complex healthcare landscape, with its vast urban centers, diverse patient populations, and intricate state regulations, requires a highly specialized approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within New York, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in New York achieve:
Pennsylvania
Why Choose MedVoice in Pennsylvania?
Pennsylvania’s diverse healthcare landscape, with its major urban centers and rural areas, along with specific state regulations, requires a robust approach to medical billing. MedVoice understands the unique payer requirements and regulatory nuances within Pennsylvania, ensuring accurate billing and unwavering compliance. Our AI-enhanced tools and experienced team help practices in Pennsylvania achieve:
View More
Alabama
Alaska
Arizona
Arkansas
California
Colorado
Connecticut
Delaware
Florida
Georgia
Hawaii
Idaho
Illinois
Indiana
Iowa
Kansas
Kentucky
Louisiana
Maine
Maryland
New Mexico
New York
North Carolina
North Dakota
Ohio
Oklahoma
Oregon
Pennsylvania
Rhode Island
South Carolina
South Dakota
Tennessee
Texas
Utah
Vermont
Virginia
Washington
West Virginia
Wisconsin
Wyoming
Our Areas of Excellence
Frequently Asked Questions
Do you work with all specialties?
Can you integrate with our existing EHR?
How soon can we go live?
Do you offer performance reports?

Services
- Medical Billing
- AI Medical Scribing
- Claims Management
- Revenue Cycle Management
AI Tools
- AI Scribe
- AI Coding Assistant
- Documentation Tools
- Compliance Monitor
